Medical Doctor Notes: What They Must Include, When to Use Them, and How to Write Them
A clinician's guide to writing valid doctor notes for work, school, disability, and return-to-work requests with fillable templates for each scenario.

Medically Reviewed by Dr. Jean-Luc "JL" Neptune, Clinical Commercial Leader
Written by the Commure Scribe Team
Published: May 8, 2026
•
9 min min read
Medical doctor notes come up in almost every outpatient setting. Yet clinicians rarely get formal training on what one should say. A patient needs a doctor note for an employer, a school, a disability office, or an insurance carrier. The clinician drafts something quickly, often from memory, and hopes it satisfies whoever is asking.
This guide covers what a medical doctor note is, when one is required, and what it must include to be valid.
What is a medical doctor note?
A medical doctor note is a signed document from a licensed physician. It verifies a patient's health status, a clinical encounter, or a functional limitation. It carries the weight of the clinician's license. It serves as a formal link between the healthcare setting and a third party. That party may be an employer, a school, a court, an insurer, or a government agency.
The term covers a wide range of documents. These include work excuse letters, school absence notes, return-to-work clearances, capacity statements, and letters that confirm diagnosis or treatment. All of them need a real clinical encounter, a licensed signatory, and language clear enough to satisfy the reader. None should disclose more protected health details than needed.
Doctor notes are not the same as chart notes or SOAP notes. Chart notes document the encounter for clinical and billing purposes. A doctor note shares a selected subset of that data with a party outside the care relationship. What gets shared depends on what the patient has approved and what the note requires.
When is a medical doctor note required?
Third parties ask for a doctor note in a defined set of situations.
Employer absence verification. Most employers need a note when an absence exceeds three consecutive days or crosses a company-defined threshold. Under FMLA, eligible employees may take up to 12 weeks of unpaid leave per year, and employers may require a completed medical certification form from the treating clinician.² FMLA uses its own form, though many employers accept a detailed doctor note as a first step.
School and university absence. K-12 schools and colleges frequently need a note after a certain number of missed days. Rules vary by district and school. Some accept a note confirming the student was ill and under a clinician's care. Others need a statement about the student's ability to return to full academic activity.
Disability and accommodation requests. Students and employees seeking accommodations under the ADA or Section 504 of the Rehabilitation Act need records of the diagnosis and its impact on daily function. According to EEOC guidance, documentation should describe the nature of the impairment, the major life activity it limits, and the functional restrictions relevant to the job or academic setting.³ Some requests also need specific recommendations. These doctor notes carry more clinical detail than a standard absence excuse.
Workers' compensation and occupational injury. After a workplace injury, the clinician must document the injury, any work restrictions, and the timeline for return to full duty. These notes feed into the workers' compensation system. They may be reviewed by an insurer, a case manager, and a claims examiner.
Return-to-work or return-to-sport clearance. Following surgery, hospitalization, or a major illness, many employers and athletic groups need written clearance before allowing full return to duty.
Court and legal proceedings. In some cases, clinicians are asked to provide records for custody hearings, personal injury cases, or disability applications. These carry the highest standards and the greatest legal risk.
What must a medical doctor note include?
A valid medical doctor note contains a minimum set of parts. Missing any of them can cause a third party to reject it, or expose the clinician to a dispute.
Clinician ID. The note must identify the author clearly: full name, credentials (MD, DO, NP, PA), practice name, address, and contact details. A signature alone is not sufficient for most recipients. It may also require the provider NPI and/or state license number.
Patient ID. The patient's full legal name and date of birth. Some schools or employers also need a medical record number or a patient ID. Do not include Social Security numbers, insurance IDs, or other identifiers that are not needed.
Date of service. When the clinical encounter occurred. If the note covers a period of illness or restriction, include the start date and the expected or actual end date.
High-level clinical overview. A brief, general statement of the condition or circumstance. Employers and schools are entitled to know that the patient had a medical reason for the absence. They are not entitled to a detailed diagnosis unless the patient consents. "The patient was seen and treated for a medical condition" is enough for many purposes. "The patient is being treated for major depressive disorder" is not needed and may create downstream discrimination risk.
Functional limitations or restrictions, if applicable. For return-to-work or accommodation notes, the doctor note should state what the patient cannot do and for how long. "No lifting over 10 pounds for four weeks" is more useful to an employer than "the patient should rest." Be clear about duration, physical limits, and any modified duty changes.
Fitness to return or projected return date. If the doctor note is clearing a patient to return, state whether they are cleared for full duty or describe modified duty. If the note covers ongoing absence, give a realistic timeline or a follow-up date.
Clinician signature. Wet or electronic signature from the treating clinician. Many institutions now accept electronically signed notes; confirm with the reader if there is any ambiguity.
Contact information for follow-up. A phone number or fax line where the employer or school can direct questions. Do not include email if the practice has not set up secure messaging for external inquiries.
What should a medical doctor note leave out?
Excessive diagnostic detail. HIPAA's minimum necessary standard applies to disclosures to third parties.⁴ Unless the patient has signed a consent for full diagnostic disclosure, stick to functional impact rather than diagnosis. "The patient has a condition that requires them to avoid prolonged standing" protects more than "the patient has lumbar disc disease with radiculopathy."
Treatment specifics. Medication names, dosages, and treatment plans are not needed on most doctor notes. Including them without written consent is a disclosure risk.
Speculation about causation. Causation opinions belong in formal workers' compensation or legal proceedings, not in routine doctor notes. If causation has been requested and the clinician has reviewed the full records, that opinion belongs in its own report. For routine doctor notes, avoid statements like "this condition was caused by the patient's working conditions." Causation claims without a full record review create legal risk.
How to write a medical doctor note: step-by-step
Step 1: Confirm what the recipient actually needs. Before writing, ask the patient who will receive the note and what it needs to say. An employer's HR department may have its own form. A university may need language about the student's ability to complete coursework. Getting this first prevents rewriting.
Step 2: Verify the encounter documentation is complete. The note should draw from a documented visit, not from a phone call or patient request alone.
Step 3: Use a template specific to the scenario. Work excuse notes, school absence notes, return-to-work clearances, and disability accommodation letters each have a different content profile. A single generic template will be suboptimal for most of them. Keep distinct templates for the most common cases in your practice.
Step 4: Write to the recipient's standard, not the chart's standard. Chart language is written for clinical readers. A doctor note for an HR department or a school needs plain language without abbreviations or clinical shorthand. Write "the patient is unable to climb stairs" rather than "pt c/o difficulty with ambulation on inclines."
Step 5: State the return date or restriction timeline precisely. Vague timelines ("the patient should rest as needed") create follow-up calls and sometimes compliance disputes. If the return date is uncertain, give a follow-up appointment date and state that a clearance letter will follow.
Step 6: Review before signing. Check that the doctor note includes all needed parts, does not share more than approved, and matches the encounter documentation. The doctor note is a legal document. It will be read by people who may act on it in ways that affect the patient's job or benefits.
Step 7: Send through a compliant channel. Fax remains the standard for most medical record transfers outside secure portal-to-portal exchanges. Unencrypted email is not a compliant channel for patient data.
Medical doctor note templates
Four fillable templates are available as separate Word documents, one for each scenario covered in this guide. Each includes labeled fields, completion notes, and a signature block. Adapt to your practice letterhead before use.
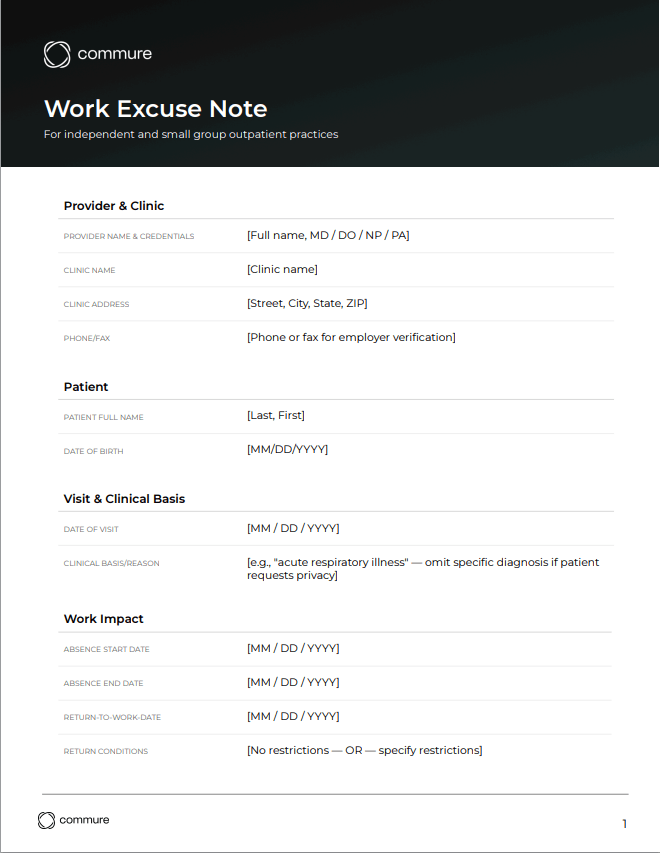
- Work excuse note: for employer absence verification
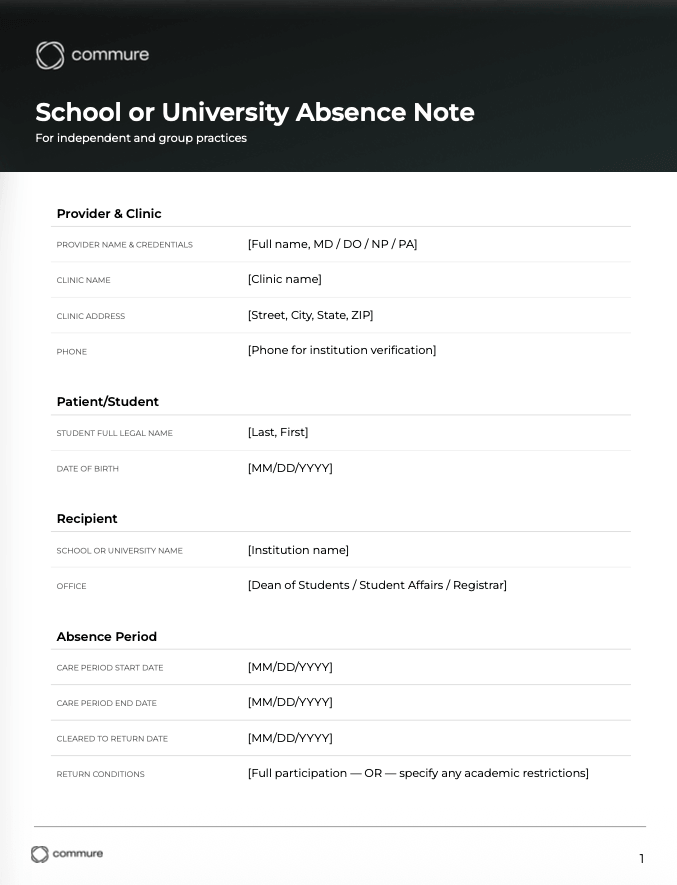
- School or university absence note: for K-12 and college absence
- Return-to-work with restrictions: for post-injury or post-illness return with modified duty
- Disability accommodation support letter: for ADA and Section 504 requests
The templates are available for download as individual files.


How do small and group practices standardize doctor note workflows?
This kind of paperwork sits outside the clinical note but depends entirely on it. In practices without a dedicated admin team, the work lands on the clinician or a single medical assistant, often without a set process.
Build scenario-specific templates in your EHR. Most EHRs support letter templates that auto-fill patient demographics, visit dates, and provider credentials. Practices that keep five to eight core templates handle most requests without writing from scratch. Useful templates include work excuse, school absence, return to full duty, return with restrictions, disability support, FMLA initiation, and a generic letter of confirmation.
Define what a completed note needs before it goes out. A short checklist covering who gets it, required parts, what can be disclosed, and send channel prevents the most common errors. This does not need to be a formal policy in a small practice. A one-page reference near the workstation where notes get drafted is enough.
Separate the generation step from the review step. Even with templates, each note needs clinical judgment. The clinician must decide what restrictions to include, what the timeline should be, and whether the encounter supports the claim. Letting support staff draft from the template and routing the draft to the clinician for review is faster than having the clinician draft from scratch. It also tends to produce a steadier output.
The friction is most pronounced where there is no dedicated staff to absorb it. A solo clinician handling their own notes, coding, and letter writing carries an admin burden that grows with patient volume. At scale within a group practice, the same gaps create inconsistency: different language, different levels of detail, different policies on what to include. A fixed process reduces that variability before technology enters the picture.
How does AI-assisted documentation affect doctor note generation?
One study of 307 primary care physicians at a large health system found a median of 36.2 minutes spent in the EHR per visit. That includes after-hours charting on top of in-clinic work.¹ Separately, AMA data shows 22.5% of physicians spend more than eight hours per week on EHR tasks outside normal work hours.⁵ Work excuse letters, return-to-work notes, and accommodation letters sit on top of that base. They are not long documents, but they need care to be accurate and legally sound.
Ambient documentation tools record the clinical encounter and generate structured notes for the clinician to review. The output, including history, assessment, plan, restrictions, and functional status, is the same content that feeds most doctor notes. When the note is complete at the close of the visit, making a work excuse or restriction letter becomes a structured task.
In practices where charting runs weeks behind, letters made from incomplete or absent chart notes carry real risk. Clinicians may not remember the exact restrictions discussed, the return date agreed on, or the exact limits the patient described. A letter made from a well-documented encounter is more accurate and easier to defend.
How Commure Scribe helps clinicians produce accurate documentation
The problem the previous sections describe, letters drafted from incomplete charts, restrictions written from memory, notes finished after hours, is a documentation workflow problem before it is a technology problem.
Commure Scribe is an AI medical scribe that records the clinical encounter and produces a structured note through a Capture, Edit, Finalize workflow. The clinician has the option to review before anything is finalized.
AI Copilot, included with the tool, draws from that note to help generate work excuse letters, return-to-work clearances, and patient-facing communications without a separate dictation step. Clinicians in family medicine, internal medicine, occupational medicine, physical therapy and other specialties, who produce restriction letters regularly, can handle encounter notes and external letters in a single workflow.
Doctor's Note Template Download
Download a copy of this template
Work Excuse Note
Click below to download
Disability Accommodation Support Letter
Click below to download
Return-to-work with Restrictions Letter
Click below to download
School or University Absence Note
Click below to download
Frequently Asked Questions
At minimum, include the clinician's name and credentials, the patient's name and date of birth, and the date of service. Add a reason for the visit, any restrictions with dates, the expected return date, and a clinician signature with contact details. Do not include more diagnostic detail than the patient has approved.
Confirm what the employer needs before writing. Use a template with the patient's name and DOB, the date of the visit, and a brief statement that the patient was seen for a medical reason. Add the start and end dates of the absence or restriction, any modified duty changes, and the return date. Sign with your full name, credentials, and practice contact details. Send via fax or a compliant secure channel.
Generally yes, if it came from a real clinical encounter with a licensed clinician who holds a license in the patient's state. Employers and schools increasingly accept telehealth-based records. Some state programs, including workers' compensation, have their own rules about in-person evaluation.
Sources
- Holmgren AJ, Hendrix N, Maisel N, et al. Electronic Health Record Usability, Satisfaction, and Burnout for Family Physicians. JAMA Netw Open. 2024;7(8):e2426956. doi:10.1001/jamanetworkopen.2024.26956 https://jamanetwork.com/journals/jamanetworkopen/fullarticle/2822959
- U.S. Department of Labor, Wage and Hour Division. "Medical Certification under the Family and Medical Leave Act." https://www.dol.gov/agencies/whd/fact-sheets/28g-fmla-serious-health-condition
- U.S. Equal Employment Opportunity Commission. "Enforcement Guidance on Reasonable Accommodation and Undue Hardship under the ADA." https://www.eeoc.gov/laws/guidance/enforcement-guidance-reasonable-accommodation-and-undue-hardship-under-ada
- U.S. Department of Health and Human Services, Office for Civil Rights. "Minimum Necessary Requirement." https://www.hhs.gov/hipaa/for-professionals/privacy/guidance/minimum-necessary-requirement/index.html
- American Medical Association. "Doctors work fewer hours, but EHR still follows them home." AMA, 2024. https://www.ama-assn.org/practice-management/physician-health/doctors-work-fewer-hours-ehr-still-follows-them- home
Try the #1 AI Scribe for Free
No Credit Card Required. Join 20,000 Clinicians.












