At the HIMSS session, “Expanding Patient Access and Reducing Costs with Interoperable AI Agents,” featuring Optimus Health Care and Commure, one theme emerged clearly: healthcare organizations are reaching a breaking point with administrative capacity.
Patient demand continues to rise, but staffing levels for call centers have struggled to keep pace, with a 35% annual turnover rate. The result is familiar across the industry: missed calls, long hold times, and administrative teams overwhelmed by routine requests.
The session explored how a new generation of AI-powered agents can scale call center capacity and improve access to care. Rather than simply routing calls or providing static chatbot responses, Commure’s Call Center Agents, part of Commure Engage, are designed to actively manage patient interactions, resolve common requests, and escalate complex situations when human attention is required. The goal is to improve patient access and experience without expanding staff.
Call Center Agents in Action
The session opened with a live demonstration of how Call Center Agents manage inbound patient calls in real time. The AI agent answers immediately, identifies the patient’s need, and guides the interaction to resolution—handling appointment scheduling, patient intake, department routing, and common questions through natural, conversational responses.
Rather than replacing staff, the agent resolves routine requests upfront, allowing teams to focus on cases that require human judgment and coordination. It can also respond to emotional cues, acknowledging frustration or discomfort, and is configurable to reflect each organization’s workflows and preferences.
The result is straightforward: calls are answered instantly, routine needs are handled without delay, and staff remain available for more complex patient interactions.
Optimus Health Care’s Perspective
For Optimus, improving patient access and operational efficiency has been a major priority. Gary Avery, Senior Director at Optimus, described the challenges many organizations face in managing high volumes of inbound patient communication.
“If patients are unhappy with long wait times and high abandonment rates, it pushes them to find another service provider.”
Research data supports this, with 60% of patients abandoning their call after more than one minute on hold, meaning answers regarding their health or next steps on care get delayed. Often, patients must make multiple calls to address a single issue.
As Gary explained, traditional call center models often struggle to keep up with peak demand. When call volume spikes, staff members are forced into a reactive posture, handling repetitive inquiries while more complex patient needs compete for attention.
AI agents offer a different model. By automating routine interactions, organizations can maintain responsiveness even during peak demand.
While earlier on in their deployment of Agents, Optimus will measure success by looking at improvements in:
- Patient satisfaction scores and feedback
- Call abandonment rates
- Scheduling and fill rates
“In order for us to continue our mission as an FQHC, we absolutely have to have patients come through our doors.”
Gary emphasized that successful AI deployment requires early involvement from a broad group of stakeholders—including front office registrars, practice managers, clinical teams, IT teams, and operational leadership—to ensure the solution reflects real workflows, incorporates staff needs, and minimizes implementation issues.
The Impact of Call Center Agents
The operational impact of AI agents becomes particularly clear when applied at scale.
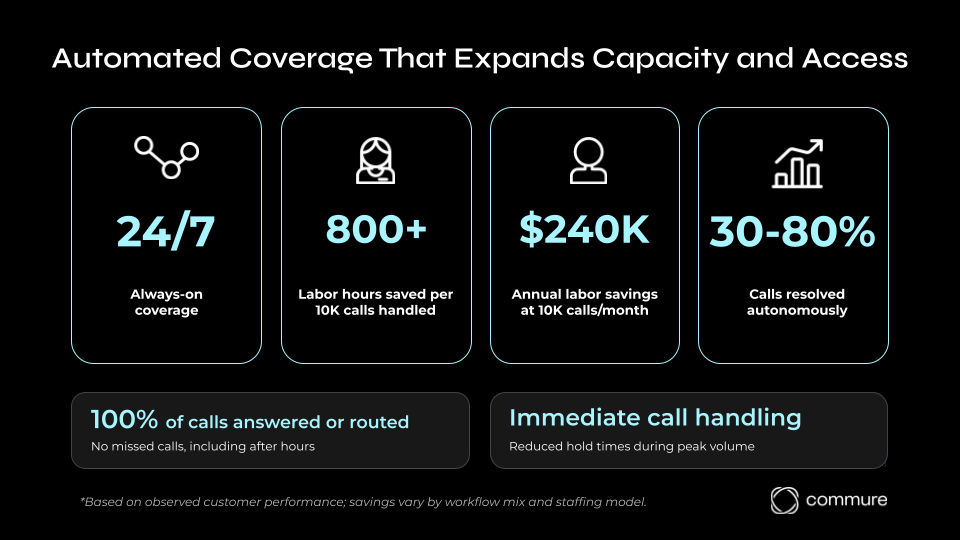
Across customer deployments using Commure Agents, organizations have observed significant improvements in how patient calls are handled. Agents provide 24/7 coverage, ensuring calls are answered even outside normal office hours.
For healthcare organizations managing large call volumes, this can translate into meaningful operational efficiency. Observed customer performance indicate:
- 800 labor hours saved per 10,000 calls handled
- $240,000 in annual labor savings at same volume
- 30-80% of inbound calls can be resolved without staff intervention, depending on workflow design
A New Layer of Healthcare Operations
The session underscored an emerging shift in how healthcare organizations think about AI. For years, much of the focus has been on clinical documentation or analytics. But AI agents represent something different: operational intelligence applied directly to the front door of care delivery. By answering calls, resolving routine requests, and routing patients efficiently, agents can extend the capacity of administrative teams while improving the patient experience.
For organizations struggling with patient access and administrative workload, the emergence of AI agents may represent one of the most practical tools available today to solve one of healthcare’s most persistent operational challenges.










.jpeg)
.jpeg)
.jpeg)



